This could lead to earlier intervention and potentially better treatment outcomes.
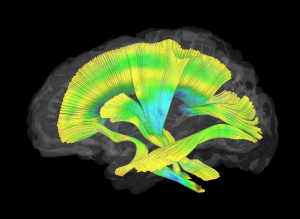
For the first time, researchers have used MRIs to show that babies with the neurodevelopmental condition fragile X syndrome had less-developed white matter compared to infants that did not develop the condition. Imaging white matter can help researchers focus on the underlying brain circuitry important for proper communication between brain regions. These findings could lead to new and earlier interventions, and potentially better treatment outcomes.
The study— co-led by University of Minnesota researcher Jason Wolff, Ph.D., and University of North Carolina-Chapel Hill researcher Meghan Swanson, Ph.D., and published in JAMA Psychiatry —shows that there are brain differences related to the neurodevelopmental disorder established well before a diagnosis is typically made at age three or later.
“Our work highlights that white matter circuitry is a potentially promising and measurable target for early intervention,” said co-first author Wolff, an assistant professor of educational psychology in the College of Education and Human Development. “These results substantiate what other researchers have shown in rodents—the essential role of fragile X gene expression on the early development of white matter.”

Fragile X syndrome is a genetic disorder and the most common inherited cause of intellectual disability in males. Symptoms include intellectual disabilities, problems with social interaction, delayed speech, hyperactivity, and repetitive behaviors. About 10 percent of people with fragile X experience seizures. About one-third of people with fragile X meet the diagnostic criteria for autism spectrum disorder.
“One of the exciting things about our findings is that the white matter differences we observe could be used as an objective marker for treatment effectiveness,” said co-senior author Heather C. Hazlett, Ph.D., assistant professor of psychiatry at the UNC School of Medicine.
For this study, Wolff, Hazlett, and colleagues imaged the brains of 27 infants who went on to be diagnosed with fragile X and 73 who did not develop the condition. The researchers focused on 19 white matter fiber tracts in the brain. Fiber tracts are bundles of myelinated axons—the long parts of neurons that extend across the brain or throughout the nervous system. Think of bundles of cables laid across the brain. These bundles of axons connect various parts of the brain so that neurons can rapidly communicate with each other. This communication is essential, especially for proper neurodevelopment during childhood.
Imaging and analytical analysis showed significant differences in the development of 12 of 19 fiber tracts in babies with fragile X from as early as six months of age. The babies who wound up being diagnosed with fragile X had significantly less-developed fiber tracts in various parts of the brain.
“It’s our hope that earlier diagnosis and intervention will help children with fragile X and their families,” said Swanson, co-first author and postdoctoral research fellow at the Carolina Institute for Developmental Disabilities at UNC. “We also hope that this knowledge might inform drug development research.”
So far, drug clinical trials have failed to demonstrate change in treatment targets in individuals with fragile X. One of the challenges has been identifying good treatment outcome measures or biomarkers that show response to intervention.
Other authors are Mark Shen, Ph.D., Martin Styner, Ph.D., and Joseph Piven, M.D., of the University of North Carolina at Chapel Hill; Annette Estes, Ph.D., of the University of Washington; Guido Gerig, Ph.D., of New York University; and Robert McKinstry, M.D., Ph.D., and Kelly Botteron, M.D., of Washington University in St. Louis.
Funding was provided by the National Institutes of Health and the Simons Foundation.
This study, which used data collected from 2008 to 2016, would have been impossible without the dedication to research from families who had another older child already diagnosed with fragile X syndrome.
News coverage
MN Daily: U of M research works toward early diagnosis for rare developmental disorder



